Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
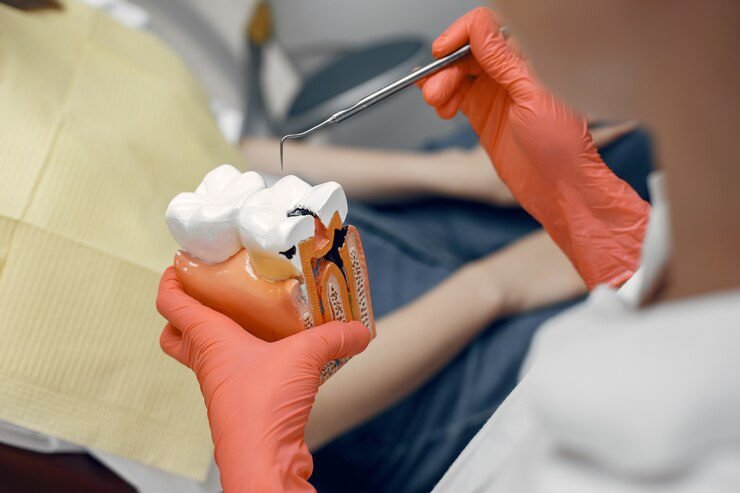
Understand how root canals work and why they don’t hurt.

Root canals are an integral part of modern dentistry, serving a crucial purpose in preserving the health and function of our teeth. By understanding the purpose of root canals, patients can alleviate any fears or misconceptions they may have. The main objective of a root canal is to save a tooth that has suffered extensive damage or infection, eliminating the need for extraction.
During a root canal procedure, the infected or damaged pulp inside the tooth is carefully removed, along with any debris or bacteria. This pulp, which consists of soft tissue, blood vessels, and nerves, can become infected due to deep decay, trauma, or repeated dental procedures. By removing the infected pulp and thoroughly cleaning the root canal system, the dentist can eliminate the source of infection and protect the tooth from further damage.
By preserving the natural tooth structure through root canal treatment, patients can avoid the potential consequences of tooth loss, such as shifting of neighboring teeth or difficulty in chewing and speaking. Additionally, root canals help maintain the aesthetic appearance of the smile by preventing the need for extraction and subsequent replacement options like dental implants or bridges.
In short, understanding the purpose of root canals allows patients to appreciate the importance of this dental procedure in saving and preserving their teeth. By seeking timely treatment, individuals can maintain a healthy and functional smile for years to come.
The key to understanding root canals lies in understanding the anatomy of a tooth. Teeth are composed of multiple layers, each serving a specific purpose. The outermost layer is the enamel, a hard and protective shell that shields the inner layers from harmful bacteria and acid. Below the enamel is the dentin, a softer layer that provides support and structure to the tooth. Lastly, at the center of the tooth lies the pulp, which consists of nerves, blood vessels, and connective tissue.
When a tooth becomes damaged or infected, the pulp can become compromised. This can happen due to deep decay, severe trauma, or repeated dental procedures. If left untreated, the infection in the pulp can spread, leading to abscesses, bone loss, and even tooth loss. Root canals are performed to remove the infected pulp and prevent further damage to the tooth. By removing the infected tissue, the dentist can save the tooth and alleviate the patient’s pain and discomfort. It is worth noting that although the pulp provides sensation and nourishment during tooth development, once the tooth is fully formed, it can survive without the pulp as it receives nourishment from surrounding tissues.
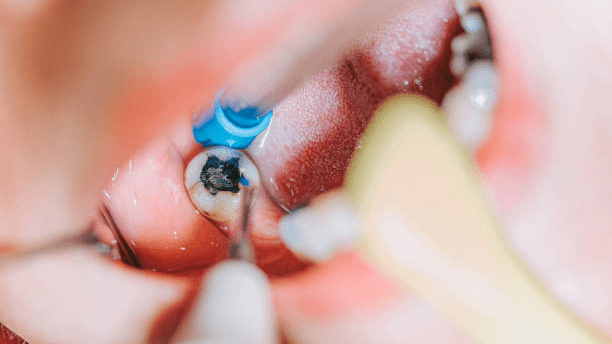
Identifying the need for a root canal is an important step in maintaining oral health and preventing more serious dental issues. There are several signs and symptoms that may indicate the need for a root canal, and it’s crucial to recognize them early on in order to seek prompt treatment.
One of the most common indicators of a potential root canal is persistent tooth pain. This pain may be throbbing, sharp, or constant, and can worsen when you bite down or apply pressure on the affected tooth. Additionally, sensitivity to hot or cold temperatures that lingers long after the stimulation has been removed could also be a red flag.
Other signs to watch out for include gum swelling, tenderness, or a small pimple-like bump on the gums near the affected tooth. These symptoms may signify an infection or an abscess in the root of the tooth, which requires immediate attention. It’s important to note that while the absence of pain or symptoms does not necessarily mean that a root canal is not needed, recognizing these warning signs and seeking professional guidance from a dentist specializing in root canal treatments is crucial to effectively address the issue and prevent further complications.
Root canal treatment, also known as endodontic therapy, is a procedure that is often necessary when the pulp of a tooth becomes infected or damaged. This treatment aims to remove the infected or damaged pulp, clean and disinfect the root canal system, and then seal it to prevent further infection or damage. The process typically involves several steps.
First, the dentist will administer local anesthesia to numb the area around the tooth. This ensures that the patient remains comfortable throughout the procedure. Once the tooth is numb, the dentist will create a small access hole in the tooth, allowing them to reach the infected or damaged pulp. Using specialized instruments, they will carefully remove the pulp from the root canals and clean the inside of the tooth to remove any debris or bacteria.
After the cleaning process is complete, the dentist will shape the root canals to prepare them for filling. This ensures a proper seal and minimizes the risk of reinfection. In some cases, the dentist may also place an antimicrobial solution inside the canals to further disinfect the area.
Once the canals are shaped and disinfected, a rubber-like material called gutta-percha is used to fill the canals. This material seals the canals and prevents bacteria from entering. In some cases, the dentist may also place a temporary filling on top of the gutta-percha to protect the tooth until a permanent restoration, such as a crown, can be placed.
It is important to note that the number of appointments required for a root canal treatment may vary depending on the severity of the infection or damage. Additionally, some cases may require additional steps, such as the use of dental posts to provide additional support for the tooth.
Overall, the step-by-step process of a root canal treatment involves removing the infected or damaged pulp, cleaning and disinfecting the root canals, and then sealing them to prevent further infection or damage. This procedure, when performed by a qualified dentist, can effectively save a tooth that might otherwise need to be extracted.

X-rays play a crucial role in root canal procedures by providing dentists with essential information about the tooth’s structure and the extent of the infection or damage. These diagnostic images allow dentists to accurately assess the condition of the tooth, identify the location of the infected or damaged pulp, and determine the most effective treatment plan.
During the initial examination, X-rays capture detailed images of the tooth roots, surrounding bone, and the pulp chamber. This helps dentists to visualize any signs of infection, such as abscesses or bone loss that may require immediate attention. Additionally, X-rays enable dentists to evaluate the complexity of the root canal procedure, such as the number and curvature of the root canals, to accurately plan the treatment and ensure successful outcomes. By relying on these precise and detailed images provided by X-rays, dentists can make informed decisions throughout the root canal procedure, ensuring effective treatment and preserving the tooth’s health.
Proper anesthesia is of utmost importance during root canal procedures to ensure a comfortable and pain-free experience for the patient. This dental treatment involves removing infected pulp from the interior of the tooth, which can cause significant discomfort if not properly numbed. Anesthesia, administered by a skilled dentist, plays a crucial role in managing pain and ensuring that the patient remains calm and relaxed throughout the procedure.
The use of local anesthesia is the most common method employed during root canal treatments. This involves injecting a numbing medication into the surrounding tissues of the affected tooth. By effectively blocking nerve signals in the area, the patient experiences minimal discomfort or pain during the procedure. A skilled dentist will carefully evaluate the patient’s pain threshold and administer the appropriate dosage of anesthesia to ensure optimal numbness and comfort. Additionally, the use of topical anesthetic gels prior to injection can help minimize any discomfort associated with the needle. In some cases, conscious sedation may also be employed to help patients with dental anxiety or those requiring more extensive treatments. The role of proper anesthesia in root canal procedures cannot be overstated, as it contributes significantly to patient comfort and the overall success of the treatment.
Here’s a structured guide outlining the importance of proper anesthesia during root canals:
| The Importance of Proper Anesthesia during Root Canals | Explanation |
|---|---|
| 1. Pain Management | – Proper anesthesia ensures effective pain management during root canal procedures, which can be complex and potentially uncomfortable for patients. |
| – Anesthesia numbs the tooth and surrounding tissues, allowing the dentist to perform the root canal without causing pain or discomfort to the patient. | |
| 2. Patient Comfort | – Adequate anesthesia promotes patient comfort and relaxation during root canal treatment, reducing anxiety and apprehension associated with dental procedures. |
| – Patients are more likely to have a positive experience and feel less stress or fear when they are comfortable and pain-free during the procedure. | |
| 3. Facilitates Efficient Treatment | – Proper anesthesia enables dentists to perform root canal treatment efficiently and effectively by ensuring that the patient remains still and cooperative throughout the procedure. |
| – With adequate pain control, dentists can focus on the technical aspects of the root canal, such as cleaning and shaping the root canal system, without interruptions due to patient discomfort. | |
| 4. Prevents Trauma and Injury | – Anesthesia helps prevent trauma and injury to the patient’s oral tissues by minimizing involuntary movements or reflex actions during root canal treatment. |
| – Without adequate anesthesia, patients may experience discomfort or pain, leading to sudden movements that could result in accidental injury to the surrounding tissues. | |
| 5. Enhances Treatment Precision | – By ensuring the patient is comfortable and pain-free, proper anesthesia allows dentists to work with greater precision and accuracy during root canal procedures. |
| – Dentists can focus on accessing and treating the root canal system thoroughly, reducing the risk of complications and improving treatment outcomes. | |
| 6. Promotes Patient Cooperation | – Adequate anesthesia promotes patient cooperation and compliance during root canal treatment, as patients are more likely to remain still and follow instructions when they are comfortable. |
| – Patients who experience minimal discomfort are more likely to cooperate with the dentist’s guidance, leading to smoother and more successful root canal procedures. | |
| 7. Supports Positive Patient Experience | – Proper anesthesia contributes to a positive patient experience by minimizing pain, discomfort, and anxiety associated with root canal treatment. |
| – Patients who have a comfortable and pain-free experience are more likely to be satisfied with their dental care and more willing to undergo necessary treatments in the future. |
Root canal therapy is a commonly used dental procedure that involves the removal and cleaning of infected or damaged pulp from inside a tooth. To effectively perform a root canal, dentists utilize a variety of specialized tools and techniques. One of the primary instruments used in root canal therapy is a dental file. These thin, flexible files are used to carefully remove the infected pulp from the root canals of the tooth. They come in different sizes and shapes to accommodate different tooth structures and ensure thorough cleaning. Dental files are designed to efficiently remove debris and shape the root canals, allowing for effective disinfection and sealing.
Another essential tool in root canal therapy is an irrigation solution. This solution is used to flush out the root canals and remove bacteria, infection, and debris. Typically, dentists use a combination of antibacterial solutions, such as sodium hypochlorite or hydrogen peroxide, to disinfect the root canals thoroughly. By irrigating the canals, these solutions help eliminate any remaining bacteria, reducing the risk of reinfection.
In addition to instruments and solutions, modern root canal therapy often involves the use of magnification devices and dental operating microscopes. These tools provide dentists with enhanced visualization of the tooth’s internal structure, allowing for greater precision and accuracy during the procedure. Magnification tools enable dentists to identify and treat even the smallest canals, ensuring a thorough and successful root canal therapy.
Overall, the tools and techniques used in root canal therapy are specifically designed to effectively clean and disinfect the root canals, ensuring optimal outcomes for patients. Dentists rely on a range of instruments, irrigation solutions, and advanced magnification tools to meticulously remove infected pulp and halt the progression of dental infections. By employing these tools and techniques, dentists can successfully save and restore the natural tooth, promoting improved oral health and overall well-being.
Root canals have long been associated with the fear of intense pain. However, it is important to debunk this myth and provide accurate information to patients. The truth is, root canal treatments do not cause pain, but rather alleviate it.
During a root canal procedure, the dentist removes the infected or damaged pulp from the tooth, which is the source of the pain. This process is performed under local anesthesia, ensuring that the patient is completely numb and comfortable throughout the procedure. In fact, a study conducted by the American Association of Endodontists found that 89% of patients reported little to no pain during their root canal treatment. This further confirms that the procedure is not a painful experience.
It is essential for patients to understand that the pain they may associate with root canals actually arises from the underlying infection or inflammation in the tooth. By addressing the root cause of the pain through a root canal treatment, patients can achieve relief and restore their oral health. It is crucial for both dentists and patients to dispel the misconception regarding the pain associated with root canals, as it can prevent individuals from seeking the necessary treatment and potentially lead to further complications.
Antibiotics play a crucial role in root canal procedures, helping to eliminate infection and promote successful healing. When a root canal is performed, it is necessary to address the underlying cause of the issue: bacteria. The dental pulp, which is located inside the tooth, can become infected due to deep decay, cracks, or trauma. If left untreated, this infection can spread to the surrounding tissues, leading to severe pain and potential tooth loss.
During a root canal procedure, the infected dental pulp is carefully removed, and the space inside the tooth is thoroughly cleaned and disinfected. This process ensures that all bacteria and affected tissues are eliminated. However, in some cases, there may still be bacteria remaining in the complex root canal system that cannot be reached by traditional cleaning methods alone. This is where antibiotics come into play.
Antibiotics are prescription medications that target and kill bacteria. They are commonly prescribed before, during, or after a root canal procedure to further prevent or eliminate any remaining bacteria. By using antibiotics, dentists can effectively reach deep within the roots of the tooth, where bacteria may have spread, and ensure that the infection is completely eradicated. This proactive approach helps to minimize the risk of reinfection and improve the chances of a successful outcome for the patient. It is important to note that the use of antibiotics in root canal procedures is carefully considered and tailored to each patient’s specific needs, taking into account factors such as the severity of the infection and the patient’s overall health.
After undergoing a root canal procedure, it is crucial to take proper care of your tooth for a successful recovery. Following the aftercare tips provided by your dentist will help ensure that your tooth heals properly and that any potential complications are minimized.
First and foremost, it is important to maintain good oral hygiene practices after a root canal. This includes brushing your teeth twice a day with a soft-bristled toothbrush and fluoride toothpaste. Be gentle around the treated tooth to avoid causing any irritation or discomfort. Additionally, flossing daily will help remove any food particles or plaque buildup that can lead to infection. Using an antimicrobial mouthwash can also provide an extra layer of protection by killing any bacteria in your mouth.
During the healing process, it is advisable to avoid chewing on the side of your mouth where the root canal was performed. This will prevent any unnecessary pressure or strain on the treated tooth. In some cases, your dentist may recommend a temporary crown or filling to provide additional support and protection while the tooth recovers.
Lastly, it is crucial to attend all follow-up appointments with your dentist. These appointments allow your dentist to monitor your progress and address any concerns or complications that may arise. By staying proactive and following your dentist’s instructions, you can ensure a successful root canal recovery and maintain your oral health in the long term.
After undergoing a root canal treatment, it is important to recognize the signs of a successful procedure. One key indicator is the relief of pain and discomfort that prompted the need for the root canal in the first place. If the toothache, sensitivity to hot or cold, or throbbing pain has significantly subsided or is completely gone, it is a positive sign that the root canal has been effective in removing the source of the problem.
In addition, a successful root canal should also result in improved oral health. This can be observed through reduced swelling and inflammation in the surrounding gum tissues. A healthy and pink gum color, without any signs of redness or tenderness, indicates that the infection has been eradicated and the healing process is underway. Moreover, if the tooth that underwent the root canal is now functioning properly, allowing you to chew and bite without any discomfort or difficulty, it further confirms the success of the procedure. Recognizing these signs can provide reassurance and confidence in the outcome of a root canal treatment.
Root canal treatments are generally safe and effective procedures, but like any medical intervention, there are potential complications that can arise. One possible complication is incomplete removal of the infected pulp tissue within the tooth. If even a small amount is left behind, it can lead to persistent infection and the need for further treatment.
Another potential complication is a missed canal. The complex anatomy of teeth can sometimes make it challenging to identify and treat all the root canals, especially in molars with multiple roots. If a canal is missed, it can harbor bacteria and cause reinfection, requiring additional treatment.
Furthermore, root canals can sometimes result in a fractured tooth. The process of removing infected tissue and shaping the root canals can weaken the tooth structure, making it more susceptible to fractures. This may necessitate further dental work, such as a crown, to restore the tooth’s strength and prevent future complications.
It is important to note that while these complications can occur, they are relatively rare. With advancements in dental techniques and technologies, the incidence of complications has significantly decreased. Your dentist will thoroughly evaluate your dental health and discuss any potential risks or complications before proceeding with a root canal treatment.
Root canals are a common dental procedure used to treat infections and save a severely damaged tooth. However, there are cases where alternatives to root canals may be necessary. These alternatives can vary depending on the specific circumstances and the patient’s overall dental health.
One alternative to a root canal is tooth extraction. In some cases, extracting the affected tooth may be the best option, especially if it is extensively decayed or damaged beyond repair. Tooth extraction may also be recommended if there is a risk of the infection spreading to other teeth or the jawbone. After the tooth is extracted, it can be replaced with a dental implant, bridge, or partial denture to restore the appearance and function of the missing tooth.
Another alternative to a root canal is a procedure called pulp capping. Pulp capping is typically done when the infection or decay has not reached the tooth’s pulp chamber. During this procedure, the dentist will remove the decayed portion of the tooth and place a protective material directly on the exposed pulp to stimulate healing. However, pulp capping is only suitable for select cases and is not as effective as a root canal in treating advanced infections or extensive decay.
It is important to note that these alternatives to root canals may not be suitable for everyone, and the decision should be made in consultation with a dental professional. Factors such as the severity of the infection, the overall dental health, and the patient’s preferences and goals will all play a role in determining the most appropriate treatment option. Seeking prompt dental care and discussing potential alternatives can help ensure the best outcome for each individual case.
The purpose of a root canal is to remove the infected or damaged pulp from the inside of a tooth, clean and disinfect the area, and then fill and seal it to prevent further infection.
The anatomy of a tooth includes the enamel, dentin, pulp, and roots. If the pulp becomes infected or damaged due to decay or injury, a root canal may be necessary to preserve the tooth and prevent the infection from spreading.
Signs that may indicate the need for a root canal include severe tooth pain, sensitivity to hot or cold temperatures, swelling or tenderness around the tooth, and darkening or discoloration of the tooth.
No, it is important to have proper anesthesia during a root canal procedure to ensure that the patient does not experience any pain or discomfort during the treatment.
Root canal therapy involves the use of specialized tools such as files, irrigation solutions, and dental sealants. Techniques like rotary instrumentation and obturation are also commonly used to effectively clean and seal the tooth.
Contrary to a common myth, root canal procedures are performed under local anesthesia, so patients should not feel any pain during the treatment. In fact, root canals are often performed to alleviate tooth pain caused by infection or decay.
Antibiotics may be prescribed before or after a root canal procedure if there is an active infection or the risk of infection spreading. However, not all root canal procedures require antibiotics, and it depends on the specific circumstances and the dentist’s judgment.
To ensure a successful recovery after a root canal, it is important to follow your dentist’s aftercare instructions. This may include avoiding chewing on the treated tooth, practicing good oral hygiene, and attending any follow-up appointments.
Signs of a successful root canal treatment include the absence of pain or discomfort, reduction of swelling, and improved oral health. Your dentist may also use X-rays to check for proper healing and the absence of infection.
While rare, potential complications of root canal treatments may include reinfection of the tooth, damage to surrounding structures, or a fractured tooth. These complications can often be prevented with proper technique and regular dental check-ups.
Alternative treatments to root canals may be necessary in cases where the tooth is severely damaged or the infection is too extensive to be effectively treated with a root canal. In such cases, tooth extraction or dental implants may be considered as alternative options.